Rhinitis
Acute rhinitis
Definition
• Acute inflammation of the nasal mucosa
• Predominantly caused by viruses (>
90 % rhino-, corona-, adenoviruses)
• Other triggers: bacterial infections, less frequently
irritative
Frequency
• Adults: 2-5 times per year
• Children: 7-10 times per year
Duration
• Usually < 4 weeks vs. chronic rhinitis
Incubation period
approx. 2-8 days
Symptoms
Sneezing, itching, congestion, obstruction of nasal breathing, excessive secretion of thick or thin mucus.
Therapy
Z. E.g. decongestant nasal sprays, inhalation, nasal rinses, glucocorticoids, antihistamines.
Concomitant diseases
• Acute sinusitis (inflammation of the sinuses)
• Acute otitis (inflammation of the middle ear)
• Acute pharyngitis (inflammation of the throat)
• Flu infection
• Acute bronchitis
Complications
Bacterial superinfection due to:
• Gram-positive bacteria: Staphylococcus aureus, Pneumococcus
• Gram-negative bacteria: Haemophilus influenzae, Proteus mirabilis, Pseudomonas aeroginosa
Vasomotor rhinitis (runny nose)
Definition
• Non-allergic, non-infectious runny nose due to
Misregulation of the nasal mucosa
• Triggers: external (mechanical, thermal or chemical) or
internal (hormonal, psychological) factors.
• Not contagious
• Determination by diagnosis of exclusion
Symptoms
• Blocked nose
• Swollen turbinates
• Watery rhinorrhoea
• Aggravated by certain odours
(e.g. perfumes, cigarette smoke, paint fumes, alcohol, strongly spiced
food, changes in temperature and air pressure, bright light).
Therapy
• Decongestant nasal sprays, z. e.g. nasic®
• Saline/dexpanthenol-based nasal sprays, e.g. nasic®-cur
• Nasal rinses (sodium chloride)
• Nasal antihistamines, e.g.
azelastine
Rhinitis allergica (Allergic rhinitis)
Definition
• Allergy: Excessive, disease-causing
specific immune reaction (= hyperergy)
against exogenous substances (= allergens)
• Sneezing, itching, runny nose
and obstructed nasal breathing
as a result of
an IgE-mediated immediate reaction
(type I allergy)
• Triggers: e.g. pollen (hay fever), house
dust mites, but also flours or chemicals
• If eyes are also affected: Allergic
rhinoconjunctivitis

Symptoms
• Eyes: tearing, redness, swelling, itching
• Nose: stuffy nose, itching, sneezing, runny nose (thin secretion).
Therapy, e.g.
• Antihistamines
• Glucocorticoids
• Specific immunotherapy
• Saline/dexpanthenol-based nasal sprays, e.g. nasic®-cur

Rhinitis medicamentosa (drug-induced rhinitis)
Definition
• Damage to the nasal mucous membrane (especially the
ciliated epithelium) with swelling and desiccation
Causes
• Excessive use of decongestant nasal sprays (rebound
phenomenon)
• Side effects of various medicines, especially certain
psychotropic drugs, antihypertensives, Rauwolfia alkaloids.
Symptoms
• Eyes: tearing, redness, swelling, itching
• Nose: stuffy nose, itching, sneezing, runny nose
(thin secretion).
Therapy
• Discontinuation of decongestant nasal sprays (in case of excessive use).
• Saline/dexpanthenol based nasal sprays, e.g. nasic®-cur
• If necessary, treat nasal congestion with glucocorticoids.
Rhinitis sicca (dry rhinitis)
Definition
• Nasal mucosal inflammation with reduced secretion production and secondary mucosal atrophy
Causes, e.g.
• Extreme temperatures
• Drug side effects
• Misuse of decongestant nasal sprays (α-sympathomimetics)
• Secretory dysfunction
• Condition after surgical interventions on the nose
Symptoms
• Dry mucosa
• Borking
• Blocked nose
• Nosebleed
Complications
• Atrophic rhinitis (Ozäna, stinky nose)
• Atrophy of the nasal mucosa
• Bacterial colonisation of the mucous membrane
• Ulceration, septal perforation
Therapy
• Keeping the nasal mucosa moist by e.g.:
• Humidifying the room air
• Saline-based nasal rinses or sprays
• Saline/dexpanthenol-based nasal sprays, e.g. nasic®-cur
• Steam inhalation
• Removal of bark, treatment of bacterial infection, surgical intervention (Ozäna)
➢ α-Sympathomimetics are contraindicated in rhinitis sicca!
Management of Rhinitis
Synergism of the combination treatment with xylometazoline and dexpanthenol


Acute rhinitis (Kehrl et al. 2003)
Results (primary efficacy parameters)
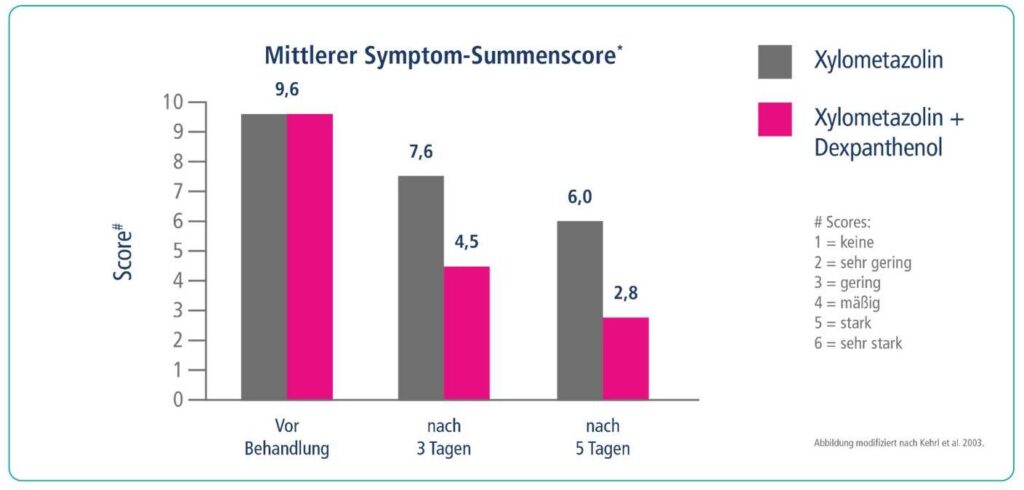
• The symptom sum score was 5.2 lower in the xylometazoline/dexpanthenol group after 3 days and 6.8 lower after 5 days, and 1.97 and 3.6 lower in the comparison group, respectively.
• The differences in the primary endpoints were found to be clinically relevant and statistically significant
• The score for nasal obstruction was 1.7, and rhinorrhoea 1.3 lower in the xylometazoline/dexpanthenol group after 5 days, and 1 and 0.9 respectively in the comparison group.
• The score for nasal mucosal redness was 1.8 lower in the xylometazoline/dexpanhenol group after 5 days, and turbinate hyperplasia was 2
lower, and 0.9 and 0.8 lower, respectively, in the comparison group
• With almost identical baseline findings, the differences between the two collectives in terms of symptom improvements by the end of treatment for the four criteria were found to be clinically relevant and statistically significant.

Conclusion: The xylometazoline/dexpanthenol combination leads to a significantly greater
reduction in rhinitis symptoms after 3 days compared to xylometazoline monotherapy.
• Scores after 3 and 5 days of treatment indicate a greater reduction in rhinitis symptoms of dryness of the nasal mucosa, bark formation, redness/inflammation of the skin at the nasal entrance and swelling of the nasal mucosa in the xylometazoline/dexpanthenol group than in the comparison group.
Conclusion
• The superiority of the combination as well as the accelerated healing are
due to the additional wound healing promoting effect of dexpanthenol
• Results indicate shorter treatment time with a reduced risk of a
“rebound effect” and improved compliance

Rationale
• Post hoc analysis of the study by Kehrl et al. 2003 on the onset of therapeutic effect and symptom freedom
Post hoc analysis of Kehrl et al. 2003
Mösges et al. 2017
Results
• The proportion of patients with no or mild rhinitis
symptoms in the xylometazoline/dexpanthenol group
was at the target parameter after 4 days:
• Rhinorrhoea 73 %, in the comparison group at 21 %.
• Redness of the nasal mucosa 79%, in the comparison group 4%.
• Nasal obstruction 80 %, in the comparison group 29 %
• Nasal concha hyperplasia 71 %, in the comparison group 29 %.

Results
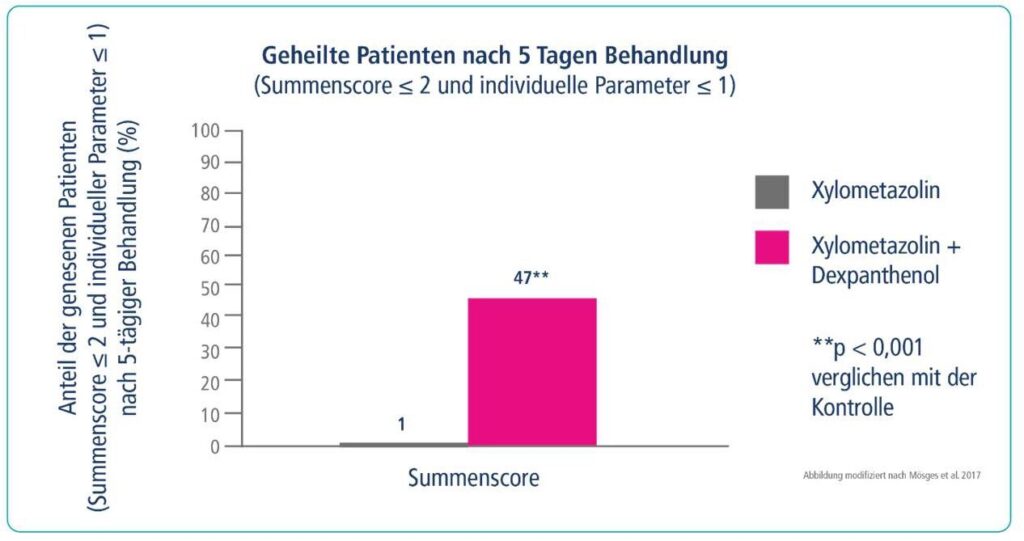
• For the sum score, “cure” was defined as a value of 2 or less, with no parameter exceeding a value of 1 (after Klimek et al. 2015)
• Under the xylometazoline/dexpanthenol combination, the proportion of “cured” patients after 5 days was 47%, while the proportion in the comparison group was 1%.